AI is transforming mental health care by introducing real-time emotional analysis into Cognitive Behavioral Therapy (CBT). This technology uses tools like voice tone analysis, facial expression tracking, and text pattern detection to monitor emotions continuously. Unlike traditional therapy, which often relies on self-reports and periodic sessions, AI offers ongoing support that can identify emotional changes as they occur. This approach helps therapists focus on complex cases while allowing users to receive timely interventions.
Key points:
- What is CBT? A therapy method aimed at changing negative thought patterns to improve emotions and behaviors.
- How AI fits in: AI tools like chatbots and wearables assist with exercises, track emotions, and provide personalized feedback.
- Real-time emotional analysis: AI evaluates emotions through voice, text, and facial cues, offering more precise insights.
- Clinical impact: Studies show AI tools improve engagement, reduce anxiety and depression symptoms, and expand access to care for underserved populations.
- Challenges: Privacy concerns, algorithm bias, and the need for long-term research remain hurdles.
AI-powered CBT is reshaping mental health care by offering continuous monitoring and tailored interventions, making therapy more accessible and effective.
The Mental Health AI Chatbot Made for Real Life | Alison Darcy | TED
sbb-itb-f5765c6
How Real-Time Emotional Analysis Works
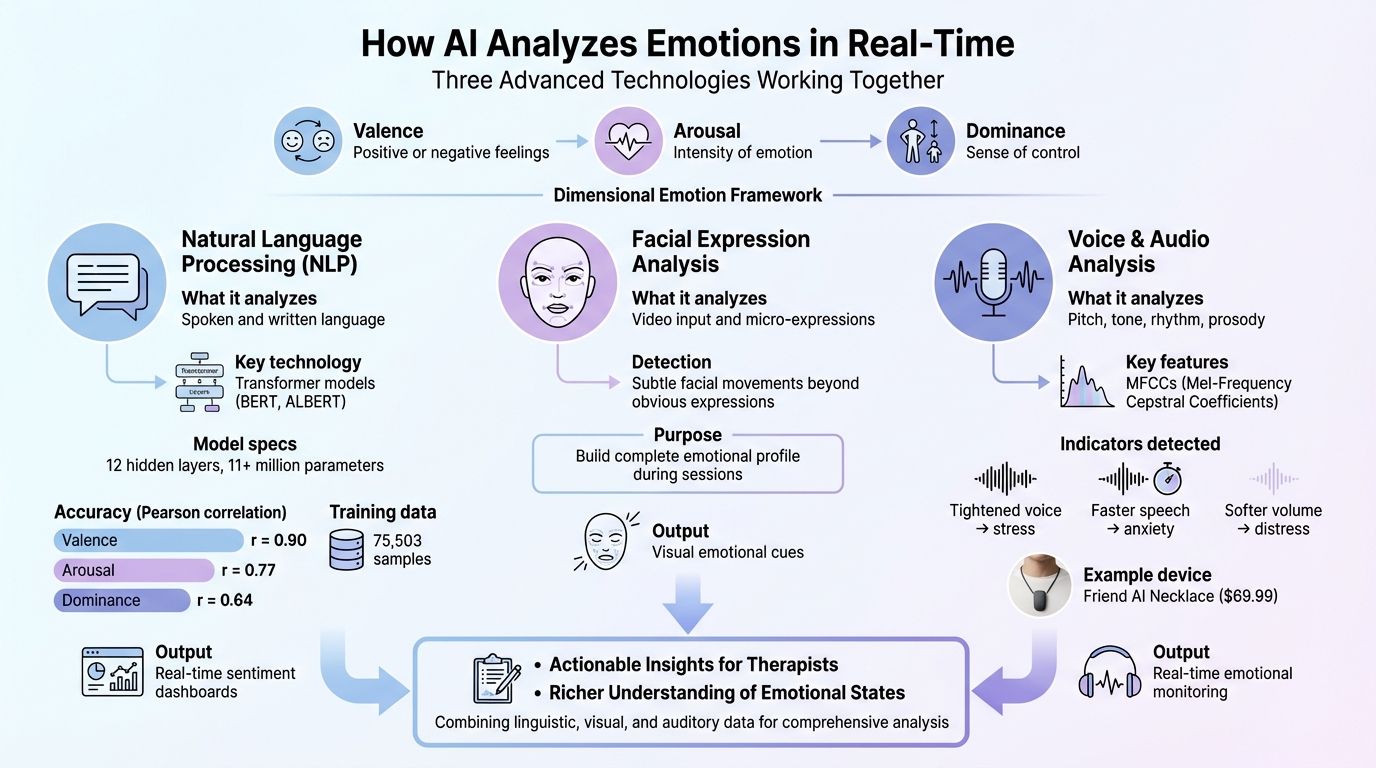
How AI Analyzes Emotions in Real-Time CBT Through Voice, Text, and Facial Recognition
Real-time emotional analysis taps into three advanced technologies to interpret human emotions with precision. Instead of relying on basic labels, it uses dimensional emotion recognition, which considers valence (positive or negative feelings), arousal (intensity of emotion), and dominance (sense of control). This approach creates a detailed emotional profile, helping therapists identify distress even when it's not directly expressed.
Natural Language Processing (NLP)
NLP dives into both spoken and written language to uncover emotional tones and detect cognitive distortions - those negative thought patterns that cognitive behavioral therapy (CBT) often targets. Transformer-based models like BERT and ALBERT map words into high-dimensional vectors, capturing subtle contextual meanings[1]. For instance, an ALBERT-based model includes 12 hidden layers and over 11 million parameters[1]. In May 2024, Julian Striegl and his team at Technische Universität Dresden developed a transformer model trained on 75,503 samples. The model achieved impressive accuracy, with Pearson correlation coefficients of r = 0.90 for valence, r = 0.77 for arousal, and r = 0.64 for dominance[2]. Tools like real-time sentiment dashboards display these emotional shifts, enabling therapists to spot unspoken signs of distress. Visual cues further complement these insights.
Facial Expression Analysis
AI also analyzes video input to detect micro-expressions - those fleeting, subtle facial movements that often go unnoticed. These tiny shifts, beyond obvious smiles or frowns, help build a more complete emotional profile during therapy sessions[3].
Voice and Audio Analysis
Emotions also leave traces in voice patterns. Pitch, tone, rhythm, and prosody all carry emotional signals. Deep learning models analyze MFCCs (Mel-Frequency Cepstral Coefficients), which are key acoustic features, to identify these emotional markers[7]. For example, a tightened voice, faster speech, or softer volume might indicate stress or anxiety. This analysis can even extend to wearables like the Friend AI Necklace ($69.99), which records and transcribes sessions for real-time emotional monitoring[6].
Together, these technologies offer therapists actionable insights in real time, enhancing the effectiveness of AI-driven interventions in CBT. By combining linguistic, visual, and auditory data, this system provides a richer understanding of emotional states.
Real-Time AI Interventions in CBT Sessions
AI is transforming Cognitive Behavioral Therapy (CBT) by delivering real-time emotional analysis and immediate interventions. These tools not only monitor emotions but also help patients apply CBT techniques right when they need them, whether during therapy sessions or in everyday life.
Cognitive Restructuring Support
AI can spot cognitive distortions through text analysis and guide users to challenge these thought patterns. For instance, Large Language Models like GPT-4 use Socratic questioning to help patients identify and rethink unhelpful thoughts. Tools like TeaBot, based on GPT-3, allow users to document distorted thoughts and work through healthier alternatives in real time[8].
A study conducted from June to July 2024 at University College London tested the Limbic Care app with 540 adults. This app used machine learning to analyze users’ emotional states and recommend cognitive restructuring exercises like digital thought records. Participants using this AI-driven tool engaged 2.4 times more frequently and had 3.8 times longer sessions compared to those using traditional static workbooks[9]. Beyond therapy sessions, wearable AI devices can detect negative thought patterns during daily interactions and suggest reframing strategies on the spot.
But AI doesn’t stop at thought restructuring - it also encourages meaningful behavioral changes.
Behavioral Activation and Goal Tracking
AI supports behavioral change by analyzing text entries and passive data from smartphones, such as GPS and accelerometer readings. This helps track whether patients are engaging in or avoiding rewarding activities[10]. Large Language Models can even assess "activation levels" from journal entries, identifying patterns of withdrawal or engagement.
Between January 2016 and November 2021, researchers at McLean Hospital and Harvard Medical School studied 38 adolescents undergoing 12 weeks of Behavioral Activation therapy. They used GPT-4o to analyze daily text entries and smartphone data, tracking participants’ mobility. Results published in October 2025 showed a strong correlation between GPT-derived activation ratings, the number of places visited, and time spent outside the home. Increases in activation were linked to higher positive emotions and reduced negative emotions[10]. AI can also suggest "Opposite Action" strategies, like encouraging someone to reach out to a friend when they feel the urge to isolate, breaking cycles of avoidance[11][12].
"Tools that assess activation between sessions could help therapists monitor treatment progress and make timely adjustments, consistent with calls for data-informed psychotherapy."
- Christian A. Webb, Associate Professor of Psychiatry, Harvard Medical School[10]
By promoting both cognitive and behavioral changes, AI tools create a more comprehensive support system. But trust is key to their effectiveness.
Creating Trust Through AI Responses
For AI interventions to work, patients must trust the system. AI builds this trust by mimicking empathy, using principles from person-centered therapy like active listening and emotionally attuned responses. By analyzing emotional dimensions such as valence, arousal, and dominance, AI provides responses that feel personalized rather than generic[1].
AI can also serve as a neutral "Artificial Third" in therapy, offering a safe, non-judgmental space for patients to share sensitive information they might withhold from a human therapist. For example, from 2024 to 2025, 104 women in active war zones in Ukraine participated in a trial using the Friend chatbot. Those who used the chatbot experienced a 30% reduction in anxiety (measured by the Hamilton Anxiety Rating Scale) and a 35% reduction on the Beck Anxiety Inventory. While human therapy showed slightly better results (45–50% reduction), the chatbot provided vital support when human therapists weren’t available[13].
Maintaining trust also requires safety measures. A "cognitive layer" that filters AI responses ensures they remain clinically appropriate and avoids harmful outputs[9]. This governance is essential for building long-term confidence in AI-driven mental health tools.
Benefits and Clinical Evidence
AI-powered CBT is making a noticeable impact on mental health outcomes. For example, in January 2026, Dr. Mirai So from Tokyo Dental College led a three-arm randomized controlled trial involving 1,187 adults who used an AI-augmented iCBT program developed by NEC Solution Innovators. The results? Participants with AI support showed a 23% higher likelihood of weekly participation compared to those using standard iCBT. At a three-month follow-up, fewer participants in the AI group had a PHQ-9 score of 10 or higher - the threshold for probable major depression - compared to the control group (difference of –0.15) [14]. These findings highlight how AI's real-time emotional insights can lead to measurable clinical improvements.
Reduced Depression and Anxiety Symptoms
AI systems excel at spotting subtle mood changes, allowing for timely and precise interventions. In a randomized controlled study involving 70 participants over two weeks, those who used the Woebot chatbot reported reduced symptoms of depression and anxiety compared to an information-only control group [1]. These reductions reinforce the role of personalized AI interactions in improving mental health.
Personalized Treatment and Better Engagement
AI-powered CBT tailors its approach to each user’s emotional state, keeping them engaged and motivated. A trial conducted in the United States between June and July 2024 compared the Limbic Care smartphone app to standard digital workbooks. Over six weeks, the AI-powered app increased engagement frequency by 2.4 times and engagement duration by 3.8 times. Exploratory analysis showed that users who followed AI-guided sessions experienced greater anxiety reduction and improved overall wellbeing [9]. Similarly, in the NEC trial, the activation of the AI's empathic feedback feature strongly predicted adherence, with an odds ratio of 9.99 [14].
"Empathic feedback emerged as a key mechanism for sustaining engagement, suggesting that AI communication may help maintain participation in scalable digital mental health interventions."
– Mirai So, MD, MBA, PhD, Tokyo Dental College [14]
Increased Access to Mental Health Care
AI-powered CBT goes beyond symptom relief and engagement by expanding access to mental health care. It offers immediate, cost-effective support, breaking down barriers for individuals in underserved areas or those stuck on long waiting lists. Additionally, the technology addresses stigma, as many people feel more at ease sharing sensitive details with an AI. While traditional unguided iCBT typically achieves remission rates of 30%–35%, AI-driven personalization is narrowing the gap toward the success rates seen with therapist-guided care [14]. Generative artificial intelligence (genAI) further enhances this potential, delivering highly engaging and tailored mental health support at scale [9].
Challenges and What's Next
AI-powered CBT with real-time emotional analysis has potential, but it faces several obstacles that need addressing before it can achieve widespread use.
Privacy, Bias, and Technical Issues
Data security is a major concern. Collecting personal information like text messages, voice recordings, facial expressions, and physiological data from wearables introduces serious privacy risks. To mitigate this, solutions such as end-to-end encryption and local-first processing - where AI operates directly on a user's device instead of relying on cloud storage - are being explored to safeguard sensitive mental health data [3][4].
Algorithmic bias and technical accuracy are equally pressing. Many AI models are trained on datasets that lack diversity, which can result in biased interpretations and reduced accuracy, particularly in uncontrolled or noisy environments. Vanessa Farsadaki, a researcher at Arizona State University, emphasizes this issue:
"Many algorithms are trained on datasets lacking demographic diversity, which can lead to biased results and reduced accuracy for certain groups"
[3]
To address this, developers need to prioritize diverse and inclusive data collection, ensuring that AI systems perform equitably across different populations. Tackling these challenges is essential for advancing the integration of AI into mental health care.
Connecting with Health Data Platforms
The future of AI-powered CBT lies in its ability to integrate with broader health systems. Platforms like BondMCP are leading this shift by merging real-time emotional data with other health metrics, such as wearable data, lab results, sleep patterns, and fitness levels. This creates a comprehensive view of both mental and physical health. For instance, emotional insights from a CBT session could inform a sleep coach, while HRV biofeedback data might trigger proactive strategies to manage anxiety before it escalates.
This integration allows for highly personalized interventions. By analyzing patterns in a user's overall health profile, AI can identify connections - like how poor sleep might increase anxiety or how specific supplements may impact mood. To enable this level of personalization while maintaining privacy, technologies like federated learning and differential privacy are crucial. These tools ensure sensitive data remains secure while still allowing for meaningful insights [5].
Need for Long-Term Research
While early results are promising, long-term studies are critical to understanding whether AI-enhanced CBT offers lasting benefits. Many existing studies are short-term, often lasting just a few weeks or months. To determine whether these interventions lead to sustained mental health improvements, there’s a pressing need for long-term randomized controlled trials. Currently, research in this field is heavily skewed, with computer science dominating (25.6%) compared to psychology (2.9%), highlighting the need for a more balanced, interdisciplinary approach [5].
Additionally, research must expand beyond English-speaking populations. Most datasets used to train AI systems come from these groups, raising concerns about the effectiveness of these tools in other linguistic and cultural settings. Without rigorous, long-term studies across diverse demographics, it's difficult to fully assess the reliability and clinical impact of real-time emotional analysis in CBT [1][5]. Continued research will not only validate current findings but also refine these tools for more precise, personalized interventions.
Conclusion: AI's Role in Mental Health Care
AI is reshaping how cognitive behavioral therapy (CBT) is delivered. Instead of relying solely on weekly sessions and patient self-reports, real-time emotional analysis enables continuous monitoring, capturing emotional changes as they occur. This evolution transforms mental health care from a reactive model to one that's proactive and preventive. Patients can now receive timely support during critical moments - like panic attacks, depressive episodes, or periods of intense stress - without waiting for their next appointment.
The data highlights this transformation. Generative AI-driven CBT apps have been shown to increase engagement rates by 2.4 times compared to traditional digital workbooks [9]. Multimodal AI systems, which blend voice, text, and physiological data, have reached up to 92% accuracy in identifying depression symptoms [15]. Dr. Mirai So from Tokyo Dental College found that AI systems providing empathic feedback significantly improved adherence, with an odds ratio of 9.99 for sustained participation [14]. These advancements mark a major step forward in mental health care delivery.
AI's potential grows even further when mental and physical health data are integrated. Mental health cannot be separated from physical well-being - poor sleep impacts mood, chronic stress affects heart rate variability, and exercise can reduce anxiety. The BondMCP - Health Model Context Protocol connects emotional insights with physical health metrics, enabling personalized care. Imagine a scenario where your sleep tracker informs your CBT app, or where emotional data influences your diet or supplement recommendations. This approach addresses the whole person, not just isolated symptoms.
However, progress comes with challenges. As Dr. Mohammad Narimani explains:
"The digital psychological signature enables dynamic and continuous detection... shifting mental health care from a reactive to a preventive paradigm" [15].
Achieving this vision requires addressing privacy concerns, eliminating algorithmic bias, and conducting thorough long-term studies. When implemented responsibly, AI-powered CBT can bridge treatment gaps, provide around-the-clock support, and adapt care to individual emotional needs.
Mental health care is evolving into a system of continuous, intelligent support. By integrating real-time emotional analysis into broader health platforms, patients gain better clarity, therapists benefit from objective insights, and the overall system becomes more accessible and effective. The tools are here - now it's about using them responsibly to make a difference.
FAQs
How accurate is real-time emotion detection in CBT?
Real-time emotion detection is making strides in AI-powered cognitive behavioral therapy (CBT). Deep learning models are becoming better at interpreting emotions by analyzing things like tone of voice, facial expressions, and behavior patterns. However, their accuracy isn’t perfect and can depend on factors such as the quality of the data, the specific context, and unique individual traits. While these tools show promise, they work best when paired with human expertise to fully understand the subtleties of emotions in therapy sessions.
Will AI emotional analysis record my voice or face?
AI emotional analysis in Cognitive Behavioral Therapy (CBT) often relies on analyzing your voice rather than capturing visual data like your face. By focusing on vocal cues, it can interpret emotions while maintaining privacy, as no facial recordings are involved.
Can AI-CBT replace a human therapist?
AI's role in Cognitive Behavioral Therapy (CBT) offers some exciting possibilities, particularly with features like real-time emotional analysis. These tools can improve mental health support by making therapy more engaging, tracking emotional and behavioral patterns, and tailoring interactions to individual needs. However, AI falls short when it comes to understanding complex emotions or providing the empathy and nuanced insight that only human therapists can offer.
There are also ethical concerns to consider, such as privacy risks and potential biases in AI systems. These issues reinforce the idea that AI should act as a complementary tool in therapy, not a replacement for the crucial human connection that therapists provide.