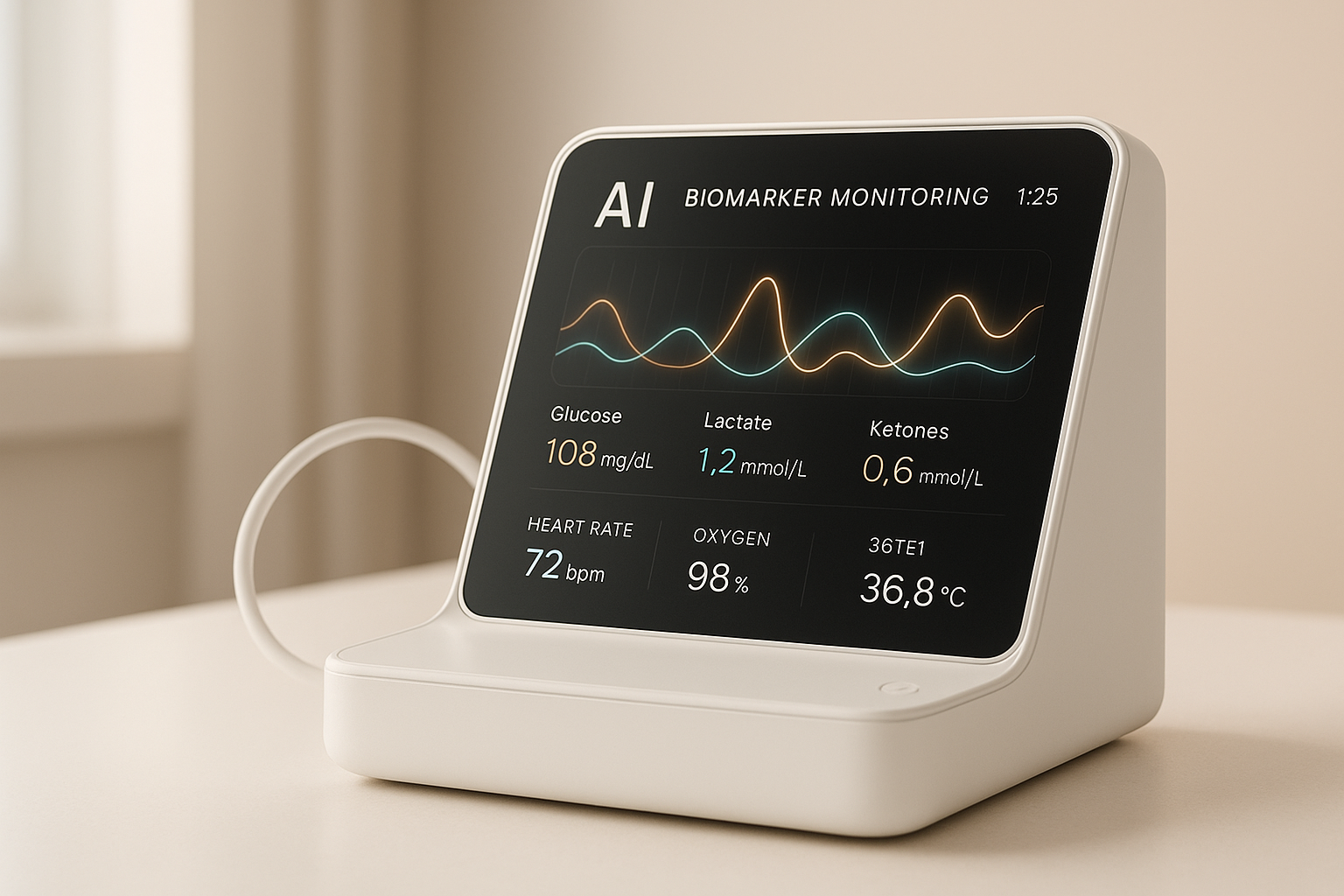
AI is transforming how we track health in real time. By combining wearable devices and advanced analytics, it turns continuous health data into actionable insights. This approach enables early detection of health changes, personalized care, and streamlined clinical workflows.
Key Highlights:
- Real-time data collection: Devices like glucose monitors and heart rate trackers provide continuous updates.
- AI-powered analysis: Identifies subtle changes in health metrics, improving diagnostics and treatment adjustments.
- Smaller clinical trials: AI reduces trial sizes by up to 70%, cutting costs and speeding up research.
- Improved patient care: Early detection of health issues and tailored interventions enhance outcomes.
- Data security concerns: Advanced encryption and compliance with HIPAA and GDPR ensure privacy.
AI-driven tools like BondMCP, Validic, and Diagnostics.ai lead this shift, offering solutions for unified health data, remote monitoring, and early disease detection. These technologies are paving the way for more efficient and personalized healthcare.
Digital Health Technology Derived Biomarkers and Outcome Assessments for Remote Monitoring
Key Features of AI-Powered Biomarker Monitoring Systems
AI-powered biomarker monitoring systems are changing the way we approach health by transforming raw data into actionable insights. These systems offer personalized solutions that guide interventions and improve health outcomes.
Continuous Data Collection and Integration
Today’s AI systems bring together data from wearables, smartphone sensors, and other devices into a single, unified health profile. Devices like heart rate monitors, sleep trackers, and glucose meters produce a constant stream of information, but traditional healthcare often struggles to process it all effectively.
In fact, 63% of adults in the US have used mobile health apps since 2022 [3]. AI simplifies the challenge by harmonizing data from multiple sources, enabling a seamless flow of information. This allows for more comprehensive baseline assessments, often incorporating detailed blood biomarker testing [1]. Unlike the occasional snapshots provided by traditional healthcare, AI tracks biomarkers over time, capturing how they change and respond to interventions.
This constant data collection enables AI to identify patterns in large datasets - patterns that might be missed during routine clinical visits [2]. By doing so, it lays the groundwork for advanced analytics that tailor health interventions to each individual.
Advanced Analytics and Personalized Recommendations
The real strength of AI-powered systems lies in their ability to turn complex health data into clear, personalized recommendations. This approach shifts the focus from generalized health management to individualized care.
AI algorithms analyze vast datasets to detect risks, suggest actions, and monitor their effectiveness [1]. For example, while standard thyroid tests consider TSH levels up to 4.5 mIU/L as normal, optimal function often falls between 1.0–2.5 mIU/L [1]. AI can identify when biomarkers fall within "normal" ranges but outside what’s optimal, prompting personalized advice for improvement.
These insights directly guide timely and specific interventions. AI can even predict how lifestyle changes - like diet or exercise - might influence biomarkers, creating a dynamic feedback loop that adjusts recommendations based on real-time results [1].
Take vitamin D as an example. While conventional ranges consider levels above 30 ng/mL sufficient, research points to 50–80 ng/mL as ideal for better immune function [1]. AI systems monitor how an individual responds to lifestyle adjustments, refining recommendations over time. This creates a system that learns and adapts to the unique needs of each person, ensuring more precise and effective health management.
Data Security and Privacy Standards
While data integration and personalization are critical, securing health data is just as important. The sensitive nature of this information makes it a prime target for cyberattacks, and the adoption of AI increases the volume and complexity of data, heightening the risk [4].
The scale of the problem is immense. Between 2005 and 2019, 249.9 million healthcare records were breached [6]. Developers are responding with robust security measures that go beyond traditional protections.
"Unauthorized access to data is the baseline [concern]. We can't even start talking about other things if we don't address that first."
– Rony Gadiwalla, CIO at GRAND Mental Health [5]
Modern AI systems employ multiple layers of security, including encryption, role-based access, and multifactor authentication, to protect sensitive data [4][7]. However, privacy challenges remain complex. A 2019 study found that AI could re-identify 99.98% of anonymized individuals using just 15 demographic attributes [4]. To counter this, developers are using advanced anonymization and pseudonymization techniques to safeguard identities while retaining the data’s usefulness for analysis [7].
Compliance with regulations like HIPAA and GDPR is critical. Regular security audits help identify vulnerabilities, and transparent policies ensure users understand how their data is being used [4][7]. The Responsible AI Framework for Healthcare (RAIFH) emphasizes privacy by design, informed patient consent, and continuous monitoring [7].
"The smallest breach could kill a business today."
– Raz Karmi, Eleos Health CISO [5]
These security measures are not just technical necessities - they are essential for earning and maintaining trust. Users need to feel confident that their sensitive health information is safe as they rely on AI-powered systems to manage their long-term health.
Top AI Tools and Platforms for Real-Time Biomarker Monitoring
AI-powered platforms are reshaping how we monitor biomarkers in real time, turning complex health data into actionable insights. With the biosensors market projected to hit $40 billion by 2026 [8], the demand for continuous health monitoring is only growing. These tools stand out for their ability to integrate data, streamline clinical workflows, and provide timely health insights.
BondMCP - Health Model Context Protocol
BondMCP tackles the issue of fragmented health data by creating a unified intelligence layer that connects all your health data sources. Using an agent-based system, it enables real-time health monitoring and decisions. Imagine your sleep tracker automatically informing your workout plan or lab results updating your supplement routine. BondMCP creates a dynamic system where your health goals guide decisions across various aspects of your life, ensuring seamless data flow for real-time adjustments.
For individuals, this means effortless automation and personalization. Instead of juggling data from wearables, lab tests, and fitness apps, BondMCP’s AI agents work together to optimize your health. It eliminates conflicting advice from different apps by providing a shared context that understands your complete health profile.
For developers, BondMCP offers a structured protocol and SDK to build health-aware, interoperable agents, cutting down development time by removing the need to create memory systems or toolchains from scratch.
Clinics and biohackers benefit from precision health delivery that ties together isolated data sources, enabling a more proactive, dynamic approach to health management. This system moves beyond static dashboards to provide real-time, responsive care.
Next, Validic takes a different approach by integrating remote patient monitoring with clinical workflows.
Validic
Validic excels in aggregating remote patient monitoring (RPM) data and integrating it into clinical workflows. It connects with over 80 EHR systems via SMART on FHIR standards, making it a practical choice for healthcare providers looking to incorporate real-time biomarker data seamlessly.
In February 2025, Validic introduced a Generative AI solution that uses Amazon Bedrock models to analyze patient trends, such as blood glucose levels, medication adherence, and lifestyle factors. This solution integrates with Epic and Oracle Health, offering clinicians a clear summary of patient data.
"Healthcare providers often face data overload from RPM platforms, but this solution changes that. Our generative AI does the heavy lifting of interpreting patient data trends, summarizing them in a way that's clear, actionable, and time-saving. This means that clinicians can spend more time focusing on patient care and less time on manual data analysis." - Drew Schiller, CEO at Validic [10]
This approach addresses a key challenge in healthcare: overwhelming amounts of data. Instead of requiring clinicians to analyze endless graphs, Validic’s AI highlights the most critical insights, reducing charting time and allowing for more patient-focused care [11].
Dr. Ron Parton, MD, MPH, highlights the impact:
"The ability for clinicians to access a concise summary of what matters most, rather than expecting them to interpret graphs and data points, is a game-changer. This innovation enables clinicians to dedicate more time to their patients, leading to stronger relationships and better health outcomes." [10]
The platform also supports cellular-enabled RPM devices and advanced sensors, ensuring reliable data collection even in areas with limited connectivity. This makes it especially valuable for patients in remote or underserved locations.
Building on this, Diagnostics.ai offers a solution focused on early disease detection through automated biomarker analysis.
Diagnostics.ai
Diagnostics.ai specializes in automated biomarker analysis, using machine learning to detect early signs of disease. By leveraging multi-modal sensor technologies, it monitors biomarkers in sweat, saliva, tears, and interstitial fluid. Its seamless integration with clinical workflows ensures both accuracy and reliability through continuous monitoring.
The platform’s strength lies in its ability to process complex biological data and identify patterns that signal early disease states or treatment responses. This provides healthcare providers with rapid insights for timely intervention. With cardiovascular diseases accounting for 31% of global deaths annually [9], early diagnosis is critical, and Diagnostics.ai helps catch potential issues before they escalate.
Its HITRUST-certified, HIPAA-compliant framework ensures the security of sensitive health data, a crucial feature for clinical applications. This shift from traditional lab-based biomarker detection to real-time automated analysis is particularly impactful in regions with limited healthcare access. Wearable IoT biomarker sensors powered by Diagnostics.ai enable continuous monitoring, offering a lifeline where traditional healthcare services are scarce.
These platforms collectively showcase how AI is transforming health monitoring, making it more integrated, efficient, and accessible. Each offers a unique solution to the challenges of real-time biomarker analysis, paving the way for better health outcomes.
sbb-itb-f5765c6
Applications and Benefits of AI in Biomarker Monitoring
AI-powered biomarker monitoring is reshaping healthcare by improving the management of chronic conditions and enabling highly personalized care. The market for AI-driven remote patient monitoring (RPM) is projected to hit $24 billion by 2033 [13], highlighting the growing importance of these technologies. These advancements are paving the way for transformative applications in patient care, offering better monitoring, tailored interventions, and enhanced engagement.
Remote Patient Monitoring
AI is making remote patient monitoring smarter by analyzing data in real time to identify trends, anomalies, and potential risks [11]. This proactive approach helps prevent costly hospitalizations and improves overall patient outcomes.
One example is Tower Health, which implemented an RPM system capable of continuous data analysis. The results? An 80% drop in overall admissions and an 84% reduction in heart failure readmissions [13]. Similarly, Stel Life used AWS technology to enhance care for underserved populations, achieving an 80% decrease in hospitalizations and boosting patient engagement [13].
"AI transforms telemedicine with improved diagnostics, real-time monitoring, and patient engagement in remote care." - ScienceDirect [12]
AI's predictive analytics take things a step further by detecting subtle biomarker changes through wearable devices and sensors. This allows healthcare providers to act early, addressing potential issues before they escalate. AI also supports medication adherence by offering personalized reminders and virtual assistant tools, while cutting administrative tasks like documentation by up to 74% [13].
In addition to monitoring, AI enables care tailored to individual needs - a topic we'll delve into next.
Personalized Health Interventions
Access to real-time biomarker data allows for dynamic adjustments to treatments, fitness routines, and lifestyle habits. AI makes it possible to fine-tune therapies without the need for frequent clinic visits, improving treatment effectiveness and minimizing side effects compared to traditional, one-size-fits-all methods [15].
A great example of this is BondMCP, which links health data to real-time interventions. For instance, it can adjust workout intensity or supplement plans based on shifts in biomarker readings.
AI also uses multimodal data - combining lifestyle details with patient-reported outcomes - to craft personalized care strategies [11]. It can identify mental health indicators and track physiological signals, providing real-time insights into pain management pathways [15]. This capability allows for quicker adjustments in pain treatments and reduces the reliance on trial-and-error approaches when prescribing medications.
Better Outcomes and Engagement
The insights generated by AI are driving better health outcomes, cutting hospitalization rates, and increasing patient involvement in their care. For instance, RPM has been shown to lower readmission rates by 76% and save around $11,472 per patient compared to traditional care methods [13]. Additionally, AI-driven RPM improves patient adherence by up to 36% [14].
Mahaska Health offers a compelling example of how AI can enhance engagement. By incorporating nurse navigators and AI-enhanced workflows into their RPM program, they improved communication and patient involvement [13]. The feedback provided by these systems encourages lasting behavior changes, empowering patients to see how their daily choices impact their biomarker profiles.
To maximize these benefits, healthcare organizations should establish strong clinical care pathways and ensure sufficient staffing to handle the demands of RPM programs [15].
Conclusion
AI-powered real-time biomarker monitoring is reshaping health care, supported by strong data and measurable outcomes.
For example, PathAI's models now surpass pathologists in identifying subtle breast cancer indicators, while Tempus uses tumor genomic profiles to guide treatments [16]. These advancements highlight the transformative impact of AI.
"The healthcare system with AI will be better than the healthcare system without it." - Friedman's fundamental theorem of informatics [17]
The global AI in healthcare market underscores this shift. Valued at $29.01 billion in 2024, it's projected to soar to $504.17 billion by 2032, with a compound annual growth rate of 44.0% [19].
Key Takeaways
AI-driven real-time biomarker monitoring enables continuous data collection, offering a dynamic and detailed view of health. It can detect subtle changes before symptoms appear, providing a proactive approach to care.
By generating personalized reference ranges, AI predicts disease onset and customizes treatments to fit individual needs [21]. It also quantifies how lifestyle changes affect biomarkers, helping users pinpoint effective strategies [20].
AI's integration capabilities address the challenge of fragmented healthcare data. Unified systems now allow sleep trackers, lab results, and fitness devices to seamlessly collaborate, enabling real-time, informed health decisions.
The financial benefits are notable too. AI has the potential to cut private payers' administrative costs by up to 20% and medical expenses by 10% [11]. For example, Abridge has reduced charting time by 74%, letting clinicians focus more on patients [11]. Such efficiencies are crucial as the healthcare sector faces a projected shortage of nearly 10 million professionals by 2030 [18].
Looking Ahead
The future of AI in healthcare looks even more promising, with innovations on the horizon poised to expand its impact.
Emerging biochemical wearables will soon monitor various markers through skin, sweat, saliva, tears, and even breath, offering real-time insights [23]. Meanwhile, multiagent frameworks - where multiple AI systems collaborate - are set to revolutionize decision-making by providing diverse perspectives on the same data [24].
For older adults, increasing passivity in data collection is a game changer. Telemedicine adoption among this group has risen to 76%, with 21% now using wearable technology to manage their health [22]. This trend simplifies health monitoring and makes it more accessible.
AI is already capable of identifying pre-diabetic trends years before traditional methods and optimizing metabolic flexibility [20]. Future systems aim to predict health issues months or even years in advance, paving the way for truly preventive care [20].
As AI becomes more integrated with digital health platforms, it will drive predictive analysis and deliver personalized interventions. This interconnected system will set a new benchmark for health optimization, where data flows effortlessly between devices and insights lead to tailored care.
This evolution shifts healthcare from reactive treatments to proactive, data-driven optimization. The tools are here, and the infrastructure is rapidly falling into place, setting the stage for a future where personalized, AI-driven health monitoring becomes the norm.
FAQs
How do AI-based biomarker monitoring systems protect sensitive health data and ensure privacy?
AI-powered biomarker monitoring systems protect sensitive health information by using strong encryption, secure storage methods, and strict access controls. These safeguards ensure that only authorized individuals can view the data, significantly lowering the chances of unauthorized access or breaches.
To further protect privacy, methods like federated learning and differential privacy come into play. These techniques enable data analysis without revealing personal records, keeping user information confidential while adhering to strict data protection laws. Combined, these measures create a secure and private framework for monitoring biomarkers in real time.
How can AI-powered real-time biomarker monitoring improve healthcare access for patients in remote or underserved areas?
AI-powered real-time biomarker monitoring is transforming healthcare for patients in remote and underserved areas by delivering timely and precise health information. This technology makes it possible to catch health issues early, manage chronic conditions more effectively, and improve diagnostic accuracy - all while reducing the need for frequent in-person visits.
By continuously tracking health data and sending proactive alerts, these tools address gaps in regions with limited healthcare resources. They lower costs, expand access to care, and enable providers to offer personalized, timely treatments - helping improve overall health outcomes for these communities.
How does AI enhance the accuracy and effectiveness of personalized health solutions compared to traditional methods?
AI is transforming personalized health care by diving deep into complex data - like medical records, lab results, and genetic profiles - to uncover patterns and deliver tailored recommendations. This approach fine-tunes treatments, boosts outcomes, and leaves patients more satisfied with their care.
Unlike older, one-size-fits-all methods, AI leverages predictive analytics and real-time monitoring to adjust treatments based on individual needs. By pulling data from various sources - wearable devices, lab tests, and even daily habits - AI paints a more complete and accurate picture of a person’s health. This allows for faster, smarter decisions, ensuring care is not only effective but also uniquely customized for each patient.