Wearable devices track more than just steps - they provide a detailed view of your health by monitoring metrics like heart rate, sleep quality, and activity levels. But without context, this data can be misleading. Context - such as time, location, personal health history, and environmental factors - turns raw data into actionable insights. For example, an elevated heart rate could mean stress, illness, or just a tough workout, depending on the situation.
Key takeaways:
- Context matters: Time of day, location, and personal health baselines shape how wearable data is interpreted.
- Better predictions: Studies show context improves accuracy in detecting health risks like stress, depression, or chronic illness.
- Integrated systems: Tools like BondMCP unify data from multiple devices, enabling personalized health recommendations.
- Applications: From heart health and sleep tracking to mental health monitoring, wearables are transforming how we manage well-being.
Wearables are evolving into smarter systems that understand your unique patterns, offering real-time, tailored advice for better health outcomes.
Situating Wearables: Smartwatch Use in Context
4 Types of Context That Shape Wearable Data
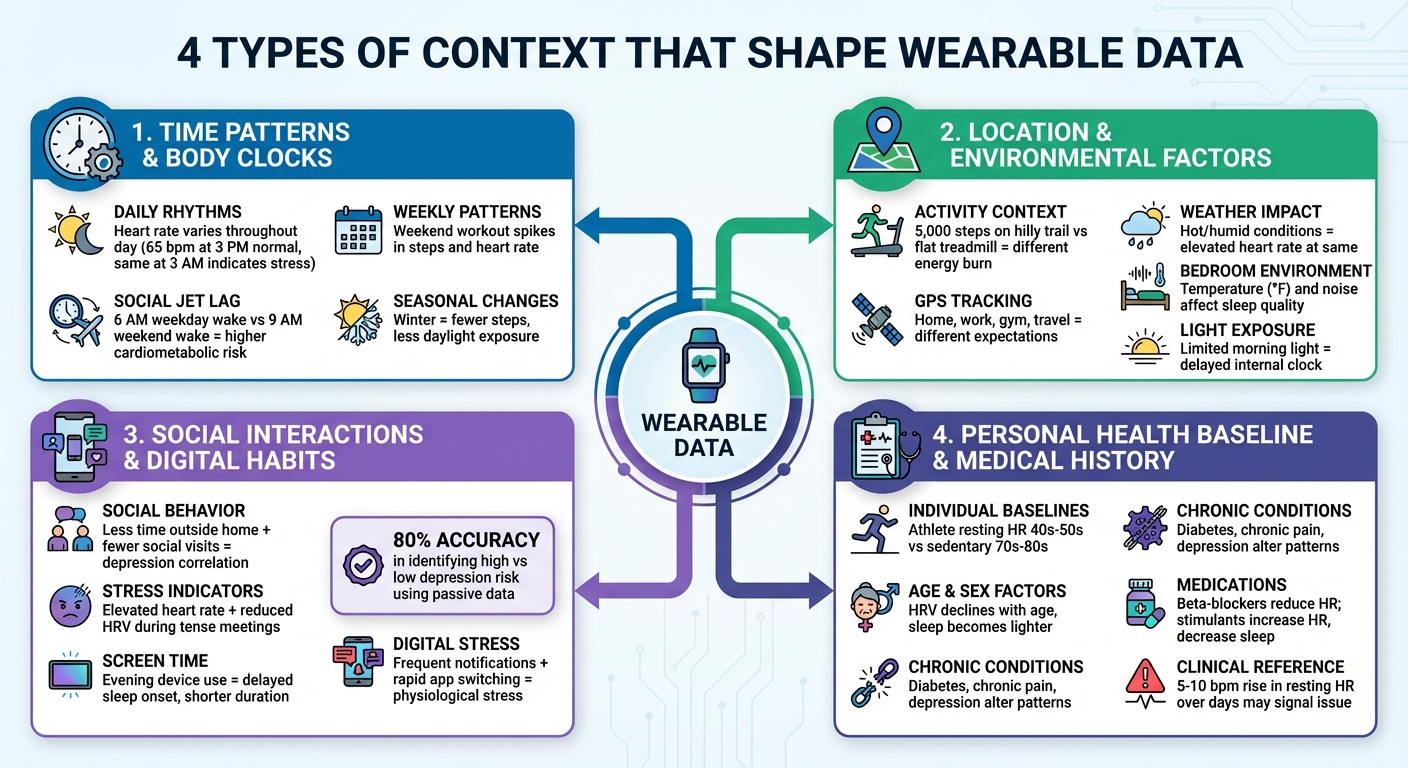
Four Types of Context That Shape Wearable Health Data Interpretation
When it comes to wearable health devices, context is everything. These tools collect a ton of raw data, but it’s the context that turns those numbers into meaningful health insights. Let’s dive into four key types of context that shape how wearable data is interpreted.
Time Patterns and Body Clocks
Your body operates on natural rhythms - daily, weekly, and even seasonal. For example, a resting heart rate of 65 bpm at 3:00 p.m. might be perfectly normal, but if you see the same reading at 3:00 a.m. while you’re asleep, it could indicate stress or illness. Metrics like heart rate, heart rate variability (HRV), body temperature, and sleep stages naturally fluctuate throughout the day.
Patterns emerge on a weekly basis, too. Weekend workouts, for instance, might cause spikes in your step count, active minutes, and heart rate. Systems that don’t account for this rhythm might label your Sunday activity as abnormal, even though it’s part of your routine. Then there’s social jet lag - when weekday and weekend sleep schedules don’t align. If you wake up at 6:00 a.m. on weekdays but sleep in until 9:00 a.m. on weekends, that shift has been linked to higher cardiometabolic risks.
Seasonal changes also leave their mark. In northern U.S. states, shorter winter days mean less outdoor activity and reduced daylight exposure. This often leads to fewer steps and more sedentary hours. A smart system would adjust activity goals during winter, rather than flagging the decrease in movement as noncompliance.
Location and Environmental Factors
Your surroundings play a huge role in shaping your wearable data. Walking 5,000 steps on a hilly trail outdoors burns more energy and elevates your heart rate compared to the same distance on a flat treadmill. GPS data helps identify whether you’re at home, at work, in the gym, or traveling - each setting comes with different activity and stress expectations.
Weather also matters. In hot, humid summer conditions, like those common in the southeastern U.S., your heart rate at a specific running pace might spike. A system that factors in local weather won’t confuse heat stress with overtraining. Even your bedroom environment, such as temperature (measured in °F for U.S. users) and noise levels, impacts your sleep. Rooms that are too warm, too cold, or noisy can lead to restless nights and fragmented sleep.
Light exposure is another critical factor. Limited morning light during winter or for those working indoors can delay your internal clock, leading to later sleep onset and grogginess in the morning. Wearables can detect these shifts and help align recommendations with your circadian rhythm.
Social Interactions and Digital Habits
Your social life and digital behavior offer clues about your mood, stress levels, and sleep quality. For instance, spending less time outside the home, visiting fewer social locations, or reducing call and text activity often correlates with worsening depressive symptoms. Similarly, elevated heart rate and reduced HRV during tense work meetings or conflict-heavy messaging are clear signs of acute stress.
Evening screen time plays a major role in sleep patterns. Using devices in the hour or two before bed is linked to delayed sleep onset, shorter sleep duration, and next-day grogginess. Wearable and smartphone integrations can even distinguish between digital insomnia (caused by screen use) and medical sleep disorders. In pilot studies, combining behavioral data like movement, phone use, and sleep patterns with self-reports has shown about 80% accuracy in identifying individuals at high versus low risk of depression [2].
Digital habits also act as stress markers. Frequent notifications, rapid app switching, and late-night work emails often align with physiological stress signals like HRV and skin conductance. Together, these data points provide a more complete picture of your mental state.
Personal Health Baseline and Medical History
Your individual health profile sets the baseline for what’s considered "normal." For example, an endurance-trained adult might have a resting heart rate in the low 40s–50s and high HRV, while a sedentary individual with cardiovascular disease may show a resting heart rate in the 70s–80s and lower HRV. Generic thresholds can misinterpret athletic bradycardia as a problem or fail to catch subtle changes that are abnormal for a specific person.
Age and sex also influence metrics like HRV and sleep. As people age, HRV tends to decline, and sleep becomes lighter and more fragmented. What qualifies as a "good" HRV or deep sleep percentage is relative to age, not an absolute number. Chronic conditions like diabetes, chronic pain, or depression further alter activity, sleep, and autonomic balance. For example, chronic pain often leads to frequent nighttime awakenings and elevated overnight heart rates - patterns that are expected for someone with that condition.
Medications add another layer of complexity. Beta-blockers, commonly prescribed for cardiovascular issues, reduce heart rate responses during exercise but may also increase sleep time. Stimulants for ADHD, on the other hand, can elevate heart rate and decrease sleep duration. Systems need to account for these factors to avoid flagging "poor fitness" or "insomnia" incorrectly. Clinical baselines, such as lab values (like A1C or lipid levels), blood pressure history, and physician diagnoses, provide a reference point for assessing risk. For instance, a consistent 5–10 bpm rise in resting heart rate over several days may signal an issue, even if it falls within population averages [1][4].
How to Add Context to Wearable Data Analysis
Combining Data Sources and Creating New Variables
To get more meaningful insights from wearable data, it’s essential to combine it with external signals that explain why the numbers look the way they do. Start by merging wearable data streams - like heart rate, HRV, steps, sleep stages, and body temperature - with external sources. For instance, enabling GPS on your wearable or smartphone can help classify your location (home, work, gym, or commuting). You can also link weather and air quality APIs to add details like local temperature (in °F), humidity, AQI, and pollen counts to your data. Integrating your calendar can help models differentiate between weekday and weekend routines, setting realistic expectations for sleep and activity. Daily check-ins capturing mood, stress, alcohol intake, or medication use can further label the data for supervised learning purposes [2][3].
Once these data sources are aligned by user ID and timestamp, feature engineering can create new variables rich with context. For example, you could calculate steps per minute based on location type (home versus work versus outdoors) or analyze HRV during sleep after travel days compared to regular days. Resting heart rate could be expressed as a deviation from a 14-day baseline, while sleep duration might be tracked on nights before early meetings versus free days. Even activity levels can be adjusted for local temperature and AQI to distinguish genuine behavior changes from environmental factors. These context-enriched variables consistently outperform raw sensor data when it comes to predicting personalized health insights from wearable anomaly data and modeling behavior changes [1][2][3].
Machine Learning Models That Use Context
Machine learning models, especially deep learning approaches like LSTM, GRU, and Transformers, shine when it comes to processing multi-channel data. These models can ingest wearable sensor streams alongside context indicators like time, location, weather, and work status, capturing temporal patterns effectively. They can also incorporate static user-level information - such as age, sex, or chronic health conditions - as part of the input. A study on depression detection using wearable time-series data showed that deep learning models outperformed traditional methods, offering high accuracy and robustness when applied to real-world datasets [7].
For classification tasks - like detecting stress, assessing relapse risk, or identifying activity types - many teams combine handcrafted context features with tree-based models such as random forests or gradient boosting. These more traditional approaches are easy to interpret, reliable, and practical for use in health apps. Including both dynamic sequences (like rolling averages or variability over daily or weekly timeframes) and static features (like baseline fitness levels, medication lists, or work schedules) allows predictions to be tailored to an individual’s habits and health profile. This combination not only improves prediction accuracy but also supports real-time, personalized recommendations [1][2][4].
Adjusting Recommendations Based on Real-Time Context
Adding context doesn’t just enhance predictions - it also improves the quality of advice users receive. By leveraging context-enriched variables, systems can deliver personalized, real-time recommendations. For example, if HRV and sleep quality drop after several nights of reduced sleep due to work deadlines, the system might suggest shorter, low-intensity workouts and emphasize naps or earlier bedtimes. When travel across time zones is detected, it could adjust sleep and activity targets while offering jet-lag advice, such as tips for light exposure or melatonin timing [2][3]. On particularly hot and humid days - common during summer in the southern U.S. - users might be advised to reduce workout intensity, exercise during cooler hours, and stay hydrated. Framing recommendations with context, like “Because you’re working a late shift tonight…” or “With today’s heat index at 95°F…,” builds trust and encourages adherence far more effectively than generic alerts [2][3].
How BondMCP Standardizes Context Integration
Standardizing context integration is crucial for cohesive health insights. Building such systems from scratch often requires rethinking data pipelines, feature storage, and agent routing for every use case. BondMCP – Health Model Context Protocol simplifies this process by offering a shared context layer and health-specific ontology that allows seamless communication between data sources like wearables, labs, supplements, fitness apps, and sleep trackers.
For users, this means your sleep tracker can inform your fitness coach, your lab results can update your supplement plan, and your long-term health goals can guide real-time decisions. For developers, BondMCP provides a structured protocol and SDK to create context-aware, interoperable, and health-savvy systems right out of the box. For clinics and health platforms, it offers a scalable way to deliver precision care by connecting siloed data, enabling proactive insights, and moving beyond static dashboards. By centralizing diverse data streams, BondMCP ensures seamless integration and context-driven insights for better health outcomes.
sbb-itb-f5765c6
Real Applications of Context-Aware Wearables
Heart Health and Metabolic Optimization
Context-aware wearables are transforming how we monitor and improve heart health. By tracking heart rate, heart rate variability (HRV), step count, and sedentary minutes, these devices can pinpoint unhealthy sitting patterns and encourage more movement throughout the day. For office workers who often sit for 8–10 hours, wearables can detect prolonged inactivity - like sitting for more than 45–60 minutes - and send reminders to stand or take a quick walk during breaks or after meetings. Research has shown that patterns of activity and mobility are better indicators of health than raw sensor data alone [1].
Timing workouts is another area where wearables shine. By analyzing sleep-wake cycles and tracking when HRV and energy levels peak - typically late morning or early evening for most adults - these devices can recommend the best windows for high-intensity interval training (HIIT). On days when sleep quality is poor or resting heart rate is elevated, wearables might suggest postponing intense exercise or opting for a more moderate activity like walking. They can also encourage short post-meal walks - just 10–15 minutes within 1–2 hours after eating - to help regulate blood sugar and support metabolic health, particularly for those managing prediabetes or cardiovascular risks [1].
These insights don’t just stop at heart health - they also pave the way for better sleep and recovery practices.
Better Sleep and Recovery Tracking
Wearables provide more than basic sleep tracking by combining metrics like accelerometry, heart rate, HRV, and respiration rate with contextual data. Factors such as time zone changes, night shifts, late-night meals, alcohol consumption, or bedroom conditions (temperature, lighting, noise) can disrupt sleep and skew heart rate patterns. Context-aware systems can label nights as "jet lag" or "environmental stress", helping users understand what’s affecting their sleep and avoid unnecessary worry [2].
For shift workers and frequent travelers, these devices offer customized sleep and recovery advice. Instead of generic "get 8 hours of sleep" tips, they might recommend gradual schedule adjustments for night shifts, blackout curtains for daytime sleep, or earlier wind-down routines before late shifts. By integrating overnight HRV and resting heart rate with the previous day’s activity and stress levels, wearables can adjust daily exercise recommendations - suggesting lighter workouts after a poor night’s sleep or encouraging more intense sessions when recovery metrics are strong [2].
Early Detection of Mental Health Changes
Wearables are also proving valuable in monitoring mental well-being. By passively tracking behavioral markers like reduced physical activity, disrupted sleep, lower HRV, irregular routines, and decreased social interactions, they can identify signs of mental health changes. For example, researchers at Nanyang Technological University developed a system that uses wearable data to predict depression risk with about 80% accuracy [2]. Higher physical activity and HRV levels are consistently linked to better mood and resilience, making them key indicators of mental health [2].
Context is crucial here to avoid unnecessary alerts. A planned vacation or rest week might naturally lead to fewer steps and less social activity, but when multiple changes - like lower movement, later bedtimes, and declining HRV - occur without a clear reason, the system can flag potential concerns. Wearables can prompt users to complete short mood assessments after nights of poor sleep or days of low activity, connecting objective changes with how they feel. This approach not only encourages self-reflection but also provides access to in-app resources or options to share data with clinicians or trusted contacts, enabling early intervention [2][4].
Clinical Use for Chronic Disease Management
The integration of wearable data into clinical care is revolutionizing the management of chronic conditions. Clinics now use these devices to monitor diseases like diabetes, heart failure, atrial fibrillation, and COPD. For instance, in type 2 diabetes, wearables can correlate post-meal walking habits, sleep duration, and heart rate patterns with glucose readings, offering tailored advice on post-meal activity and evening routines. In heart failure, tracking daily step counts, heart rate, and sleep quality can detect early signs of worsening health - such as declining activity levels and increasing resting heart rate - prompting timely medication adjustments or clinic visits [1][3].
A system called BondMCP – Health Model Context Protocol is making this integration more seamless. By combining wearable data with electronic health records, medication lists, lab results, and patient-reported outcomes, BondMCP allows healthcare providers to see the full picture rather than isolated metrics. Dashboards summarize trends alongside contextual details like work schedules, travel, and seasonal changes, enabling personalized coaching, medication adjustments, and goal setting. This approach moves beyond static data, offering continuous, context-rich insights that support proactive care for chronic disease management [1][3].
Building Systems That Use Context-Rich Data
Data Structure and Cross-Platform Compatibility
Wearable devices like Apple Watch, Fitbit, Garmin, and Oura all track health metrics, but they use different terminology and methods for things like sleep stages, heart rate variability (HRV), and activity types. Without a standardized system, a "high-intensity workout" from one brand might not align with a "vigorous run" from another, even if they're essentially the same activity.
To solve this, a unified data model is key. By creating a standard schema - mapping data into universal categories like ActivitySession, SleepEpisode, and HeartRateSeries - we can make these metrics comparable across devices. For example, steps can be recorded as integers per minute, heart rate in beats per minute, and timestamps in ISO format with clear time zones. This consistency allows for cross-device analysis and insights.
A large-scale behavioral model trained on over 15 billion hourly measurements from 162,000 participants proves how powerful this approach can be. By combining higher-level metrics like activity, sleep, and HRV with raw sensor data, the model achieved strong predictions for 57 different health tasks [1].
The BondMCP – Health Model Context Protocol takes this a step further by offering a shared structure for health data. BondMCP’s standardized event model allows seamless integration of data from wearables, smart devices, and apps. For instance, if a sleep agent detects "late caffeine intake + evening high-intensity workout + high bedroom temperature", it can treat these as combined risk factors for poor sleep - regardless of which device or app provided the data. This unified structure ensures consistent and actionable insights across platforms.
Beyond making data compatible, this approach lays the groundwork for strong privacy protections.
Privacy and Data Protection
While context-rich data offers valuable insights, it also raises serious privacy concerns. Detailed behavioral and location data can inadvertently reveal sensitive information, such as home addresses, workplaces, or visits to clinics or support groups. Even anonymized data can sometimes be re-identified, exposing personal details like mood, pregnancy status, or chronic health conditions.
To address these risks, on-device processing and federated learning are essential tools. Devices can analyze raw data locally to generate features like "late-night screen time" or "weekend bedtime drift", and then share only aggregated scores or alerts with servers. Federated learning takes this a step further by training global models directly on individual devices, sharing only gradient updates instead of raw data. For example, mental health researchers using this method have achieved 80% accuracy in predicting depression risk, all while keeping sensitive app usage and GPS data private [2].
Other safeguards include data minimization, which means collecting only what’s necessary for the task at hand. For example, raw GPS data can be converted into categories like "home", "work", or "gym" before storage. Strong access controls, end-to-end encryption, and clear consent processes are also critical. Users should know exactly what data is being collected, why, and how long it will be retained. In the U.S., systems must comply with HIPAA and state privacy laws, which grant users the right to access, delete, or opt out of data sharing.
While privacy is crucial, systems also need to cater to local preferences and usability standards.
Adapting for U.S. Users
For U.S. users, systems must reflect local measurement preferences: distances in miles and feet, weight in pounds, temperature in °F, and dates in the MM/DD/YYYY format with a 12-hour clock (AM/PM). Internally, timestamps should still be stored in UTC with linked local time zones to handle issues like time zone changes or daylight saving time. This ensures that metrics like sleep patterns and work schedules remain accurate, even when users travel.
Context models should also account for U.S. lifestyle factors. For instance, car dependency in many areas means fewer incidental steps compared to walkable cities. A sudden drop in step count during a snowstorm or around Thanksgiving should be flagged as an environmental factor, not a health concern. Recommendations should align with U.S. guidelines, such as aiming for 7,000–10,000 steps per day, 150 minutes of moderate exercise per week, and typical work hours from 8:00 AM to 5:00 PM. Tailoring feedback to these norms ensures that it stays relevant and practical for daily life in the U.S.
Through these technical and privacy measures, systems can deliver precise, meaningful recommendations that fit seamlessly into everyday American routines.
The Future of Context-Aware Wearables
In the next ten years, wearables are expected to transform into sophisticated health systems that adapt to your individual needs - taking into account your baseline health, surroundings, and medical history. Forget the generic "10,000 steps" goals; instead, algorithms will use wearable data combined with factors like your work schedule, weather conditions, medication timing, and lab results to determine your ideal sleep, training, and recovery targets.[1][3] Foundation models, trained on over 15 billion hourly measurements from 162,000 participants, have already shown that analyzing higher-level behavioral patterns - like activity rhythms, mobility trends, and cardiovascular changes - provides better health predictions than relying solely on raw sensor data.[1] As more contextual data is integrated, these systems will shift toward real-time personalized health optimization, moving away from one-size-fits-all averages. This progress also addresses a major hurdle: fragmented data.
The biggest challenge to this vision is data fragmentation. Right now, disconnected devices often provide conflicting advice, leaving users overwhelmed. BondMCP tackles this issue by unifying wearables, lab results, medications, and interventions through a shared intelligence layer. Its health-specific ontology and context framework allow AI agents to "speak the same language." This means your sleep data can seamlessly adjust your workout plan, lab results can refine your supplement routine, and your long-term health goals can guide your daily choices - all happening behind the scenes.
For U.S. consumers, this evolution means having a continuous health co-pilot that offers clarity, customization, and automation. Developers gain access to BondMCP’s structured SDK, which simplifies building context-aware health agents without needing to reinvent core components like memory or routing. Clinics and health platforms benefit too, as BondMCP enables precision health at scale, integrating previously siloed data to support proactive, risk-based care instead of the usual episodic visits.[5][6] As context-aware wearables become more common, the systems that thrive will be those that unify data, safeguard privacy, and deliver real-time, reliable insights that both users and healthcare providers can depend on.
The future of wearables lies in making data work together seamlessly. With BondMCP setting the bar for health optimization, the next generation of devices is poised to fulfill the promise of personalized, context-driven health management.
FAQs
How does understanding context improve the accuracy of wearable health data?
Wearable health devices become far more effective when they consider the context behind the data they collect. For instance, they can distinguish whether an increased heart rate is due to physical activity or stress, offering insights that are much more relevant to your health.
By factoring in elements like your location, current activity, or even the time of day, AI can sift through routine fluctuations and hone in on the signals that really matter. This approach results in tailored recommendations that better align with your daily habits and personal health objectives.
What factors help wearables better understand your behavior?
Wearable devices become much better at understanding your behavior when they take into account important contextual factors like your surroundings, social setting, and physical condition.
For instance, environmental details - such as temperature or air quality - can shed light on shifts in your activity levels. Similarly, your social setting, like working out solo versus with a group, can impact how you perform. On top of that, physiological data, including your heart rate or sleep patterns, allows wearables to offer advice and insights tailored specifically to you.
By combining these layers of context, wearables go beyond just crunching numbers. They provide insights that feel more relevant and practical, aligning with the way you live your life.
How do wearables assist in identifying early signs of mental health changes?
Wearable devices are proving to be valuable tools in spotting early signs of mental health changes. By tracking sleep quality, activity levels, heart rate variability, and mood-related patterns, they can paint a picture of behavioral trends. When paired with information about a person’s surroundings, this data can uncover potential signs of stress, anxiety, or depression before they become more serious.
When wearable data is combined with advanced systems like AI, users can benefit from customized insights and timely interventions that align with their daily habits and environments. This forward-thinking approach helps individuals manage their mental health more effectively while promoting overall well-being.
