AI health agents are transforming how personal and clinical health data is managed. Memory systems enable these agents to track your health journey over time, offering tailored advice based on your evolving needs. Here's what you need to know:
- What It Does: These agents monitor health data like sleep, fitness, medications, and lab results, providing personalized insights by "remembering" past interactions.
- Why It Matters: Memory ensures consistency in long-term health tracking, improving decision-making and avoiding redundant or conflicting advice.
- How It Works: Four types of memory - working, episodic, semantic, and procedural - store short-term data, health history, medical facts, and task workflows, respectively, following secure agent memory protocols.
- Key Features:
- Hierarchical Systems: Organize data into layers for faster and more accurate retrieval.
- Hybrid Architectures: Combine vector databases and knowledge graphs for better reasoning.
- Shared Context Layers: Allow multiple health tools (e.g., wearables, fitness apps) to work together seamlessly.
Building Agents That Learn: Managing Memory in AI Agents
sbb-itb-f5765c6
Core Components of Memory Architecture in Health Agents
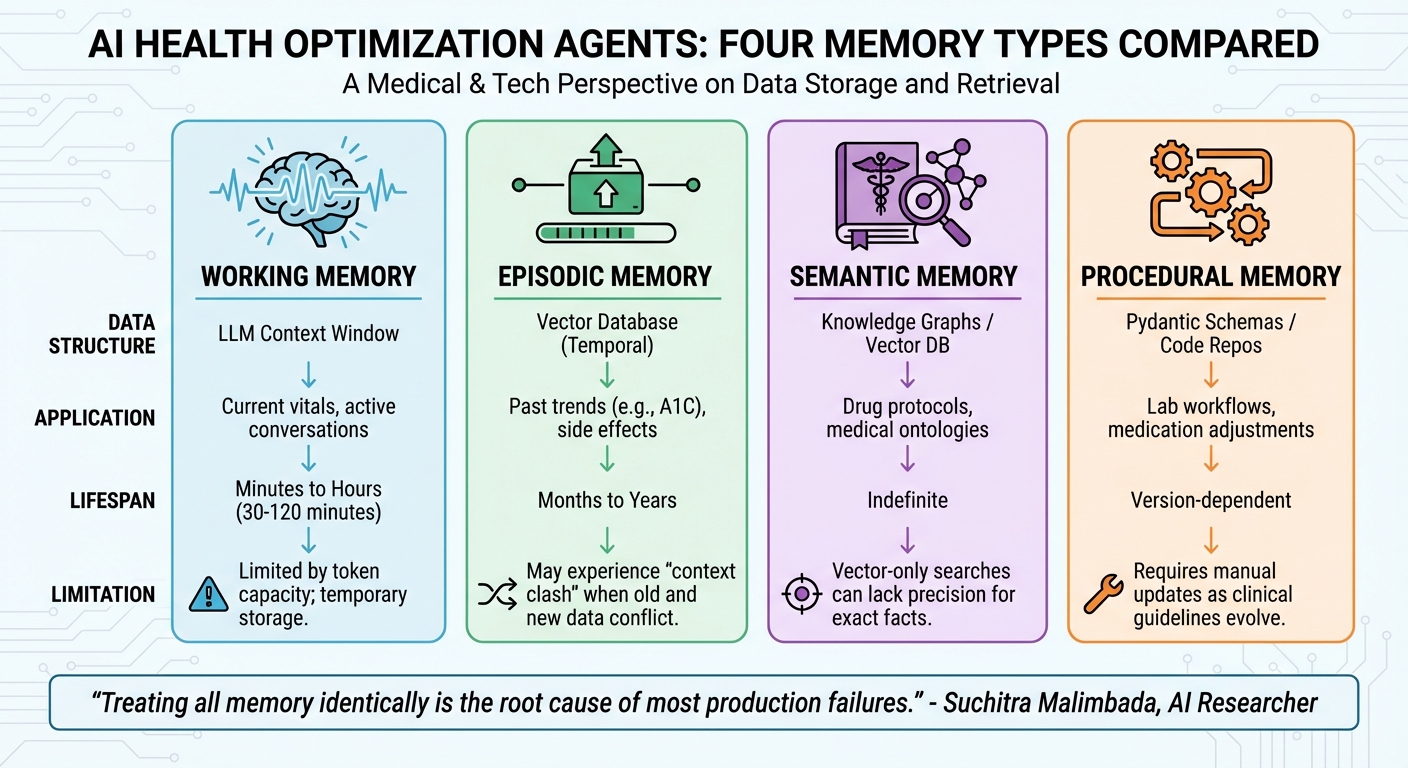
Four Types of Memory in AI Health Agents: Functions, Lifespans, and Limitations
Health optimization agents rely on four key memory types that mimic how human cognition works. Let’s break them down:
- Working memory is like the agent's short-term workspace. It temporarily holds data such as current vitals and recent sensor readings. This memory operates within the LLM context window and typically lasts between 30 and 120 minutes before being cleared or archived [5].
- Episodic memory serves as a "flight recorder" for your health history, capturing events in chronological order. For example, when your agent recalls you mentioned sleep issues three weeks ago or tracks your A1C trends over the past six months, it’s pulling from this memory. Episodic memory is stored in a vector database designed to index events over time [4].
- Semantic memory is where the agent stores medical facts that don’t change - things like drug interaction databases, treatment guidelines, or ontologies like SNOMED CT. While episodic memory focuses on historical events, semantic memory is all about established knowledge [4].
- Procedural memory encodes step-by-step instructions for performing tasks. For instance, when an agent orders labs using HL7/FHIR APIs or adjusts a medication dose based on a protocol, it’s relying on procedural memory. This type of memory is often stored in code repositories or schemas (like Pydantic) that define exact workflows [4][1].
These memory types form the foundation for the advanced systems discussed in the next section.
Hierarchical and Hybrid Memory Architectures
To manage and analyze this data efficiently, agents use hierarchical systems and hybrid architectures.
Hierarchical systems, like H-MEM, organize data into layers such as Domain, Category, Memory Trace, and Episode. This setup acts like a filing system, helping agents retrieve specific data without wasting time scanning through irrelevant information. By avoiding "context distraction", these systems ensure that critical health signals don’t get lost in the noise. For instance, the ENGRAM memory system outperformed full-context baselines by 15 points on the LongMemEval benchmark while using just 1% of the tokens [3].
On the other hand, hybrid architectures combine the speed of vector databases with the precision of knowledge graphs. Vector databases excel at quickly finding semantically similar information, like a past discussion about fatigue. However, knowledge graphs enable more complex reasoning, such as identifying dangerous drug interactions across a patient’s medication history - something a simple similarity search might miss [4].
Take MemGPT, for example. It uses an operating system-like paging mechanism to move data between a small "Core Memory" (active context) and a much larger "Archival Memory." This approach cuts token costs by over 90% compared to less efficient methods [4]. Similarly, BondMCP integrates a shared context layer, allowing different agents - like a sleep tracker and a training coach - to seamlessly share insights. This unified memory system ensures that all health data stays interconnected, enabling better decision-making.
Memory Types Compared: Use Cases and Limitations
Each memory type plays a specific role in health optimization, but they also come with certain trade-offs. Here’s a quick comparison:
| Memory Type | Data Structure | Application | Lifespan | Limitation |
|---|---|---|---|---|
| Working | LLM Context Window | Current vitals, active conversations | Minutes to Hours | Limited by token capacity; temporary storage [4][5] |
| Episodic | Vector Database (Temporal) | Past trends (e.g., A1C), side effects | Months to Years | May experience "context clash" when old and new data conflict [4][5] |
| Semantic | Knowledge Graphs / Vector DB | Drug protocols, medical ontologies | Indefinite | Vector-only searches can lack precision for exact facts [4][5] |
| Procedural | Pydantic Schemas / Code Repos | Lab workflows, medication adjustments | Version-dependent | Requires manual updates as clinical guidelines evolve [4][5] |
"Treating all memory identically is the root cause of most production failures." - Suchitra Malimbada, AI Researcher [4]
In practice, these memory systems work together to deliver personalized, real-time health insights. For example, in 2025, the MCP-AI architecture managed a 58-year-old patient (ID: MCP-CHRONIC-225) with Type 2 Diabetes. The system used episodic memory to aggregate wearable data and glucometer logs, semantic memory to store metformin dosing guidelines, and procedural memory to execute lab orders. By pulling from the right memory type at the right time, the agent ensured accurate and efficient decision-making across long-term health workflows [1].
How Long-Term Memory Works in Health Systems
Long-term memory in health systems is all about keeping track of what’s important over time. Whether it’s monitoring a patient’s decade-long battle with diabetes or ensuring seamless coordination between specialists, these systems are designed to remember key details, discard irrelevant data, and make everything easily accessible when needed.
Clinical Systems and Longitudinal Patient Memory
In clinical settings, long-term memory functions like a “black box” for patient care. Take the MCP-AI architecture, validated in December 2025, as an example. This system created protocol-driven memory objects that pulled together data from a variety of sources - caregiver interviews, EEG waveforms, genetic tests, wearable devices, and glucometer logs. It also preserved the reasoning history behind diagnostic and treatment decisions. This means clinicians could review the logic behind past actions, avoid losing critical context during handoffs, and validate or adjust future patient-centered treatment plans seamlessly [1].
These protocol-driven memory objects are essentially version-controlled files that capture a patient’s state, clinical goals, and the reasoning process behind decisions. The MCP-AI research team described its impact like this:
"MCP-AI transcends simple task optimization, it revolutionizes the manner in which AI understands, structures, and participates in care delivery, utilizing traceable and interpretable reasoning logic" [1].
While clinical systems thrive on detailed, long-term records, consumer health agents face the challenge of synthesizing diverse data streams in real time.
Personalized Health Optimization Agents
Consumer health systems, on the other hand, need to piece together data from various personal sources - wearables, lab results, coaching logs, supplement plans, and fitness routines - all in real time.
The Mnemosyne architecture, tested through blind evaluations, excelled at this task, achieving a 65.8% win rate for realism and memory compared to the standard 31.1% [7]. What set it apart? Mnemosyne uses graph-structured memory, which stores clear relationships between entities. Instead of merely recalling that you mentioned fatigue three weeks ago, it links that fatigue to your iron levels, sleep patterns, and workout intensity.
This enables what’s called multi-hop reasoning. For instance, if your sleep tracker shows you’re only getting six hours of rest per night, your lab results reveal high cortisol levels, and your training log indicates five days of intense workouts, the system can connect the dots. It might suggest that overtraining is affecting your sleep and stress hormones - something a basic search wouldn’t catch [4].
Advanced systems also incorporate temporal encoding to differentiate between outdated and current health data. SynapticRAG, for example, embeds timestamps directly into its vector representations. This ensures it won’t recommend an old medication dosage or reference obsolete health goals [4].
Shared Context Layers for Multi-Agent Systems
Bringing it all together, shared context layers allow multiple health agents to exchange data seamlessly across the health continuum. Instead of each tool - like your sleep tracker, nutrition app, and fitness planner - operating in isolation, they all contribute to and draw from a unified source of truth.
BondMCP exemplifies this concept. Acting as a shared context layer, it enables different health agents to stay synchronized with your full health history without duplicating effort. For example, if your sleep tracker detects poor recovery, it updates the shared context layer so your fitness planner can automatically adjust your workout intensity. Similarly, if lab results show a vitamin D deficiency, your supplement plan updates instantly.
This approach eliminates redundant work and prevents conflicting recommendations [4]. It also ensures reasoning continuity during transitions. If you switch from working with a general health coach to a metabolic health specialist, the new agent inherits the complete reasoning history and contextual markers from past recommendations - saving time and avoiding the need to start from scratch [1].
Memory Management and Safety Techniques
In health AI systems, managing memory goes far beyond just storing data. It’s about making smart decisions on what to save, what to discard, and how to safeguard everything in between. A poor approach can lead to bloated databases, conflicting recommendations, or even security breaches. On the flip side, a well-thought-out strategy ensures systems remain efficient, accurate, and dependable.
Memory Encoding and Retrieval Methods
Health systems rely on hierarchical memory architectures to organize data into different levels of abstraction. For example, systems like H-MEM process queries through structured layers such as Domain, Category, Memory Trace, and Episode. This prevents the system from scanning all available data and helps avoid "context poisoning", where unrelated information clouds the results [4].
Hybrid vector-graph systems blend two powerful retrieval approaches. Vector-based retrieval excels at finding conceptually related information, while Knowledge Graphs (GraphRAG) enable multi-step reasoning. For instance, analyzing drug-to-drug interactions requires the system to trace explicit relationships between medications - something vector search alone struggles to accomplish [4][5].
To handle time-sensitive data, temporal indexing integrates timestamps directly into vector representations. This ensures the system doesn’t confuse, say, your current medication dosage with one from six months ago. Tools like SynapticRAG use this strategy effectively [4][7]. Similarly, weighted knowledge graphs rely on Exponential Weighted Average (EWA) to prioritize recent data, resolving potential contradictions [6].
These structured techniques lay the groundwork for smarter memory management and pruning.
Autonomous Memory Management
Health AI systems must determine which memories to keep and which to let go. RIF scoring - which evaluates Recency, Relevance, and Frequency - helps identify data worth retaining, keeping databases streamlined [4].
Inspired by the Ebbinghaus Forgetting Curve, systems adopt cognitively inspired forgetting to prune rarely accessed data. Research shows this can shrink vector databases by 40% to 60% within 30 days of operation [4].
To keep working memory efficient, step-boundary summarization condenses information at task completion. Instead of holding onto every detail from a lengthy interaction, the system extracts the key points and discards the rest [5]. For short-lived data, a Time to Live (TTL) mechanism, ranging from 30 to 120 minutes, ensures sensitive information doesn’t linger unnecessarily [5].
By managing memory this way, systems not only improve efficiency but also enhance safety and performance.
Privacy and Compliance in Health Memory Systems
Beyond memory encoding and management, secure data handling is critical in health systems. One key practice is the removal of personally identifiable information (PII) and sensitive credentials before storing data [5]. Stripping out this information early minimizes risks in the event of a breach.
The Model Context Protocol (MCP) offers a version-controlled framework that captures clinical objectives and decision histories in auditable files. This approach aligns with FDA Software as a Medical Device (SaMD) guidelines and HIPAA requirements, ensuring transparency and compliance. As the MCP-AI research team explains:
"MCP-AI provides a scalable basis for interpretable, composable, and safety-oriented AI within upcoming clinical environments" [1].
Instead of permanently deleting forgotten memories, compliant systems use tiered archival storage. Data is encrypted and securely archived, meeting legal hold requirements while keeping active databases uncluttered [4]. To add an extra layer of safety, physician-in-the-loop verification allows clinicians to review and approve AI-generated plans through interactive dashboards before they’re implemented [1][2].
BondMCP exemplifies these principles through its shared context layer, seamlessly integrating memory management, retrieval, and privacy safeguards across health agents. By standardizing how data is encoded, accessed, and protected, it enables multiple agents to collaborate effectively without compromising security or compliance.
Future Directions and Challenges
As memory systems for health agents continue to evolve, several hurdles stand in the way. Key areas of focus include scaling systems without losing precision, unifying data from various sources into coherent patient profiles, and establishing ethical standards for data retention. These challenges are critical for the future of health-focused AI.
Scalability and Multi-Agent Coordination
Expanding structured memory systems brings its own set of difficulties, especially when it comes to managing increased data volumes without sacrificing performance. For multi-agent setups, shared team memory plays a crucial role. Clear rules for promoting information - from individual to team to organizational memory - help agents collaborate effectively while avoiding duplication and maintaining data privacy [5].
Systems like MemGPT tackle this issue with virtual context management. By using an operating system-style paging system, MemGPT moves data between a small "Core Memory" (active context) and a larger "External Context" (archival storage). This method cuts token costs by over 90% compared to approaches that rely on full conversation histories [5][4]. Selective forgetting techniques further optimize storage. For instance, the ENGRAM architecture surpassed full-context baselines by 15 points on LongMemEval, all while using only about 1% of the tokens [3].
Personalization and Multi-Modal Integration
Bringing together data from legacy electronic health records (EHRs) and modern wearables is no small feat. It requires standardized interoperability and rigorous data cleaning. Healthcare generates around 30% of the world’s total data volume, and the global big data healthcare market is expected to grow nearly fivefold, surpassing $255 million between 2023 and 2030 [11][12].
One of the biggest challenges lies in legacy systems. Many EHRs were originally designed for billing purposes rather than long-term research [10][11]. Standards like FHIR and HL7 are essential for smooth data exchange, while cloud-based data warehousing offers the scalability needed to handle complex, high-volume data streams [11][13].
BondMCP provides an example of how to address these integration issues. Its shared context layer and health-specific ontology enable agents to combine structured EHR data with unstructured inputs, such as wearable data and lab results, into a unified vector space. This approach eliminates the need to redesign memory management for every new application, streamlining the process of integrating diverse data sources.
As technical barriers are overcome, it will be equally important to develop ethical and governance frameworks to guide these advancements.
Ethics and Governance in Long-Term Memory
As health agents become more autonomous, ethical considerations must keep pace. Issues like consent for long-term data retention, rights to delete memory, and addressing algorithmic bias are critical. Systems must adhere to FDA Software as a Medical Device (SaMD) guidelines, which emphasize transparency in decision-making processes [1].
The MCP-AI research team highlights the importance of traceability:
"The architecture aligns with key principles of FDA Software as a Medical Device (SaMD), including the ability to track changes in AI behavior over time, support version control, and provide transparent documentation of decision-making processes" [1].
Unlike opaque neural systems, protocol-driven designs log every step of reasoning - what was inferred, which data was referenced, which modules were used, and which clinical thresholds were applied [1]. Privacy filters and user models must also be incorporated to determine what information is stored permanently (e.g., family history) versus temporarily (e.g., casual conversations) [9][15]. Physician oversight and ethical data retention practices will remain essential.
As Cell Reports Medicine notes:
"Successful and equitable integration hinges on navigating these profound technical, ethical, and regulatory hurdles" [14].
These principles are critical for delivering the continuous, personalized care that advanced memory architectures promise. The emergence of multi-agent systems and the concept of an "AI Agent Hospital" - where specialized agents work together through shared memory layers - will require robust governance to ensure equitable healthcare delivery and maintain patient trust [14][8].
FAQs
How do memory architectures enhance decision-making in health optimization agents?
Memory systems play a crucial role in enabling health optimization agents to make smarter, more tailored decisions by providing both context and continuity. Short-term memory (STM) focuses on recent data - like vital signs, workout logs, or sleep metrics - ensuring recommendations remain consistent during a single interaction. On the other hand, long-term memory (LTM) retains historical data, trends, and user preferences over time. This allows agents to detect patterns, such as shifts in glucose levels, and craft more personalized interventions.
When STM and LTM work together, agents can merge real-time inputs with past insights to deliver highly accurate, context-aware recommendations. Take BondMCP as an example: it integrates data from wearables, lab results, and individual goals into a unified system designed to enhance health outcomes. This memory-centric approach ensures that every decision is informed, customized, and easy to understand, helping users improve their health without added complexity.
How do hierarchical and hybrid memory systems enhance AI health agents?
By combining short-term (session-level) and long-term (persistent) storage, hierarchical memory systems empower AI health agents to handle immediate conversations while keeping essential patient information - such as medical history, lab results, and lifestyle habits - securely stored. This dual approach ensures interactions are quick and focused, while also enabling personalized care that evolves over multiple sessions.
Hybrid memory systems take this a step further by merging symbolic representations (like diagnoses or medication schedules) with vector-based embeddings, which capture intricate patterns from unstructured data such as sensor readings or clinical notes. This setup provides two major benefits: it offers clear, auditable insights for clinicians and leverages advanced pattern recognition to identify trends, such as sleep irregularities or glucose fluctuations. The result? Enhanced accuracy, fewer errors, and clinically useful recommendations that can be acted upon with confidence.
When these memory systems are implemented within frameworks like BondMCP, they enable seamless data sharing and collaboration between AI agents. This ensures real-time, personalized health management that’s not only efficient but also scalable and secure.
How do AI health agents protect personal data and comply with privacy regulations?
AI health agents are built with privacy and compliance at their core, incorporating robust security measures to protect sensitive health data. Information is encrypted both when stored and during transmission, ensuring its safety. Access is tightly controlled through role-based permissions, limiting who or what can view or modify specific data. Additionally, every interaction - whether it's reading or updating a record - is meticulously logged, creating a detailed audit trail. These practices align with regulatory standards like HIPAA and FDA guidelines for software-as-a-medical-device (SaMD).
To safeguard user permissions, consent management systems are in place to record and enforce user preferences. Data-sharing is handled using standardized formats, such as HL7/FHIR, to minimize unnecessary exposure. Protocol-driven frameworks like the Model Context Protocol (MCP) further bolster security by automating processes like encryption, de-identification, and access control. This layered approach not only reduces the likelihood of data breaches but also ensures compliance with privacy laws like HIPAA and GDPR. As a result, AI health agents can confidently provide personalized, context-sensitive health recommendations while maintaining strict data protection standards.
